PCOS – Who? What? When? How? Why?
An attractive 29 year old girl (slightly overweight with some acne) and been married for 2 years. She spends half the day with children in a nursery (She’s teaches at the nursery) and yearns to have children of her own. She has been trying to conceive and has visited a gynaecologist . The reports are normal barring a diagnosis of PCOS.
What is PCOS ?
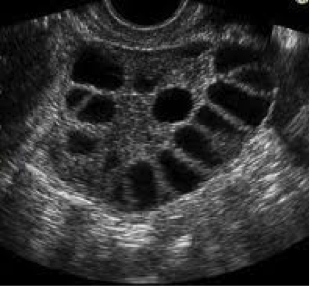
Polycystic ovary syndrome (PCOS) is a common condition that affects the way your ovaries work. In the UK, about seven in every 100 women have PCOS. If you have PCOS, your ovaries may have many small cysts or follicles (small, fluid-filled lumps) on them. Your ovaries may also be larger than usual.
Ovaries are small organs located inside a woman’s abdomen (‘tummy’). Eggs (ova) mature here and are released about once a month. This is called ovulation. Ovaries also produce the hormones (chemicals) oestrogen, progesterone and testosterone.
Before ovulation, the egg develops in a small swelling on your ovary called a follicle before it’s released. A number of follicles begin to develop but only one will become a fully mature egg. If you have PCOS, many more follicles than usual start to grow, but none of these develop into an egg for ovulation. These follicles become cysts that stay on your ovaries.
That being said the presence of cysts does not always confirm a diagnosis of PCOS which may be present sans cysts.
PCOS affects each woman differently. Symptoms include the following—-
- Having irregular periods or no periods at all.
- Problems with fertility (you need to ovulate to become pregnant and you may not be ovulating regularly).
- Being overweight or have problems losing weight.
- Having more hair than usual (hirsutism) on your face, around your nipples or on your lower abdomen.
- Thinning of the hair on top of your head.
- Oily skin or acne.
What goes wrong in PCOS patients –
- Mature egg is not formed in time
- If a mature egg is formed the chances of it being poor quality are high
- Miscarriage rates are high
Management
- Step 1 : diagnosis of PCOS can be confirmed by an ultrasound scan. Several hormone imbalances mimic PCOS like Thyroid hormone imbalances and so it is important to exclude alternative diagnoses
- Step 2: An insulin resistance test needs to performed (IRT)
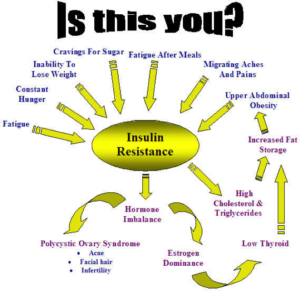
PCOS and insulin resistance are frequently found together, which makes it important to understand this common problem. Insulin is a hormone which is produced by the pancreas, a gland in the abdomen with a lot of functions. It is typically secreted in response to a large amount of glucose , or sugar, in the blood. Once produced, insulin causes glucose to be taken into the body cells to be used for energy. Women with PCOS frequently have insulin resistance , meaning their body does not respond as quickly to insulin. The sluggish response will cause larger and larger amounts of insulin to be required before glucose is taken into the body tissues, and eventually a change in the way the body deals with sugar. Consistently high levels of glucose in the blood can lead to diabetes. In the years before actually being diagnosed as diabetic, known as pre-diabetes, a number of physiologic changes occur within the body. During this stage, which can last as long as 10 to 12 years, women frequently do not experience any of the symptoms found in diabetics. The body is no longer as sensitive to insulin as it may have been before. This leads to high blood sugars after eating that do not quickly lower. Because PCOS is now recognized as a risk factor for developing diabetes, it is recommended that women with the disease be routinely screened so that insulin resistance can be found early, and treatment can be initiated earlier.
- Step 3 : according to IRT results doses of metformin should be titrated to bring insulin levels under control
- Step 4 : Weight, diet and lifestyle control. Women can conceive naturally by just losing weight.
- Step 5 : If a woman is unable to conceive spontaneously after controlling her insulin levels she should consult an infertility specialist as she would most probably require assisted reproductive techniques.
 WHAT IS THE RECOMMENDED MEAL PLAN FOR PCOS?
WHAT IS THE RECOMMENDED MEAL PLAN FOR PCOS?
Currently there is no scientific evidence to support one particular diet for PCOS. Evidence-based recommendations suggest that women with PCOS should focus on balance and moderation. Recommended lifestyle changes include:
- Weight loss of 5-10% if overweight or obese in 3 months.
- Decreased caloric intake if weight loss is desired.
- Decreased intake of enriched carbohydrates.
- Increased fiber intake including fruits, vegetables, and beans.
- Decreased fat intake, particularly saturated fat.
- Smaller, more frequent meals (every 3-4 hours) to help control blood glucose levels.
- Balanced meals including carbohydrates, protein, and fat.
- At least 150 minutes of moderate or vigorous activity per week for diabetes prevention.
KEY POINTS TO REMEMBER

- Avoid all junk food
- Consume a wide variety of whole foods
- Foods in their most natural form (fresh, frozen, or dried).
- Fruits, vegetables, beans, legumes, whole grains, fish, lean meats, nuts, and seeds should be eaten daily.

About Author:
Dr. Swarno Rekha Kazi
General Practitioner
